Is Dry Needling Safe? What to Expect at Your First Session
Honest answers on dry needling safety, side effects, and what actually happens in your first session — from a Petaling Jaya physiotherapist.
A patient messaged me before her first appointment. She'd been referred for dry needling for a stubborn upper trapezius problem — six weeks of massage and stretching, no lasting change. She wanted to come in. But she also wanted me to know, upfront, that she was not great with needles.
That message is more common than people think. I'd rather answer it honestly before you're lying on the treatment table.
So: is dry needling safe? For most people, when done by a trained physiotherapist, yes. The longer answer involves a few things worth knowing before you book.
What dry needling is (briefly)
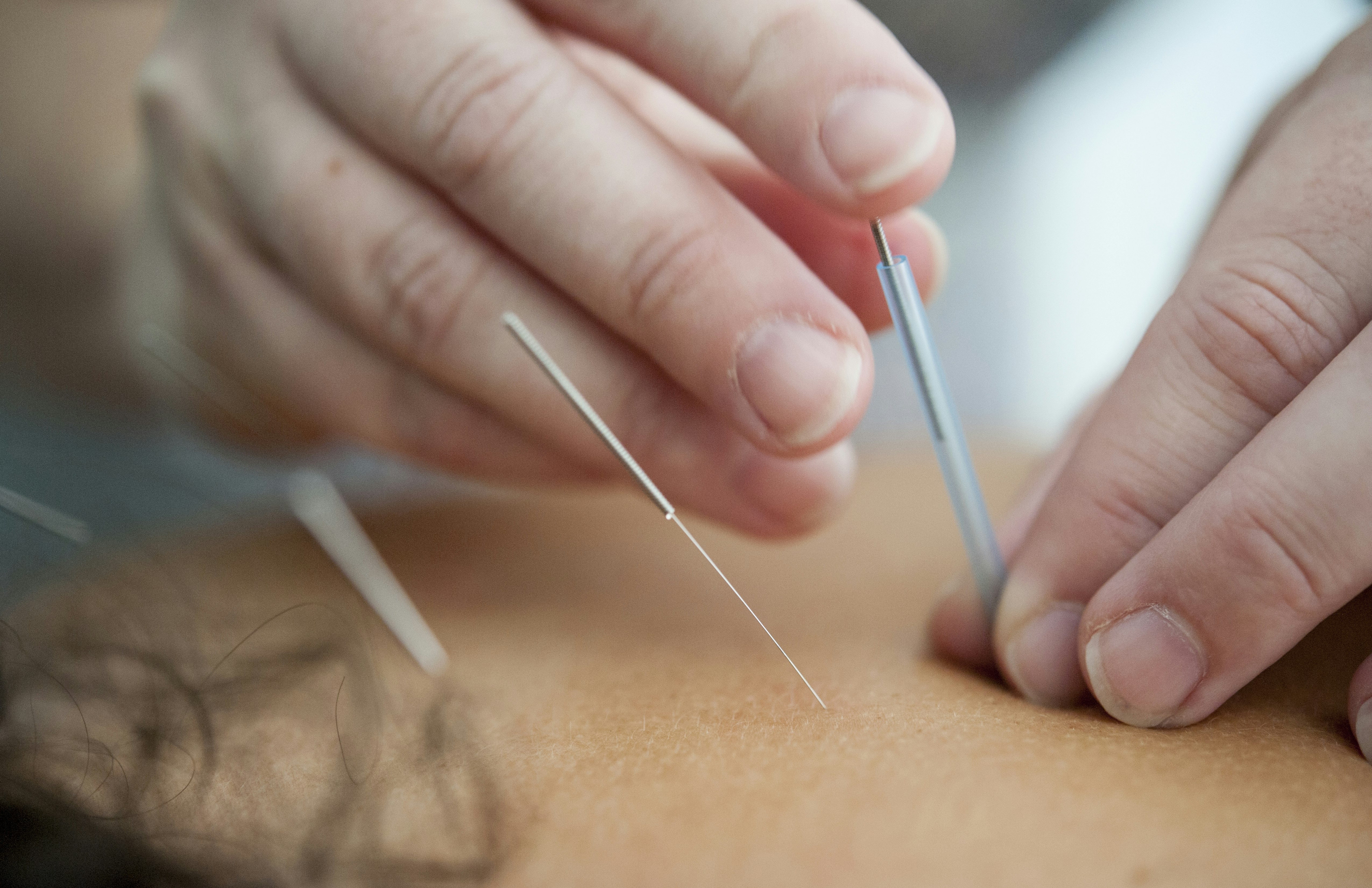
If you want the full explanation, I've written about it in detail in Dry Needling vs. Acupuncture: A Malaysian Physio Explains. The short version: a thin sterile needle is inserted directly into a myofascial trigger point — a tight, hypersensitive knot in muscle tissue. No medication. The needle mechanically disrupts the trigger point, producing a local twitch response that releases the muscle and resets its neurological firing pattern.
It's grounded in Western anatomy and neurophysiology, not Traditional Chinese Medicine. The needles look similar. The target and the reasoning are different.
The honest safety profile
Dry needling has a strong safety record when practised by clinicians trained in anatomy and needling technique. But "safe" doesn't mean "without any effects," and I think patients deserve a clear picture.
The most common side effect is post-needling soreness. Most patients get it. It feels like the muscle soreness after a heavy gym session — peaks around 24 to 48 hours and resolves on its own. For some patients it's barely noticeable; for others it's significant for a day. I tell everyone to expect it and to treat it with gentle movement and heat, not rest.
A vasovagal response — lightheadedness, brief faint — is uncommon but real, particularly in anxious patients or those who haven't eaten. I keep patients lying down for this reason and monitor through the session. If you've fainted during blood draws before, tell me before we start.
Minor bruising or local bleeding can occur at needle sites. It's occasional, usually small, resolves in a few days. More likely around superficial muscles or small surface vessels.
Serious complications — pneumothorax and nerve injury are the two most commonly raised — are rare and prevented by proper training. Needling near the thoracic spine and ribcage carries theoretical pneumothorax risk; a trained clinician uses specific angles and depths that avoid it. I'm not going to tell you the risk doesn't exist, but it is essentially theoretical when you're working with someone who has done the training properly. Needling a nerve produces a sharp electric sensation — we stop immediately if that happens.
As for contraindications: dry needling isn't appropriate for everyone. Patients on blood thinners need careful discussion first. Local skin infection, open wounds at the site, significant immunocompromise — all ruled out. During pregnancy, certain areas are avoided. And if needle phobia is at the level where lying still isn't possible, we start somewhere else. More on that below.
What actually happens at your first session
The first thing we do is assess. Where the needles go isn't simply determined by where it hurts — it's determined by where the dysfunction is. That means looking at your movement patterns, palpating for trigger points, and reasoning through the muscle chains contributing to the problem. A shoulder complaint might lead me to work on the neck. A knee issue might involve the hip. Needle placement follows the clinical picture.
Once that's done, I explain what you're about to feel. There are two main sensations: a dull, deep ache when the needle reaches the trigger point, and sometimes a brief twitch — a quick involuntary jump of the muscle. That twitch isn't a problem; it means the needle has found what we're looking for. Patients usually describe it as surprising more than painful. The ache while the needle is in place tends to feel like pressure, heaviness, or a dull throb — not the sharp sting of an injection.
Dry needling at this clinic is part of a broader physiotherapy session, not a standalone procedure. Depending on what we're treating, it's combined with manual therapy, exercise prescription, or other techniques. The needling component typically takes ten to twenty minutes within the session.
After: expect the soreness. Keep moving — light activity is better than sitting still. A heat pack over the area in the evening helps. Avoid intense exercise on the treated area for the first 24 hours.
On needle phobia
Dry needling needles are very thin — the same gauge as acupuncture needles, substantially finer than any injection or blood draw needle. No hollow bore, no liquid, no plunger. The sensation is genuinely different from what most needle-phobic patients are bracing for.
Most patients who tell me they're needle-phobic tolerate dry needling once they understand what it actually involves. The anxiety usually comes from associating it with blood draws and injections — and that association doesn't hold here.
If your anxiety is severe — if the idea alone produces a significant stress response — we don't have to start there. There are other effective techniques I can use first, and we can work toward dry needling gradually once some trust has been built. I'd rather take an extra session to get there than have a difficult experience that puts you off something that could genuinely help.
Before you book
If you have specific questions — a medication you're on, a condition you want to flag, or just wanting to talk through the anxiety before committing — send a message first.
WhatsApp Felicia directly and we can have that conversation before you're on the table.
Pinpoint Physiotherapy & Rehabilitation offers dry needling in Petaling Jaya at our Oasis Square clinic in Ara Damansara.
Related articles.
If this piece helped, these will too.

Pain After Dry Needling: Why You Feel Worse Before You Feel Better
Woke up more sore after dry needling? Here's exactly why that happens, what's normal, what isn't, and how to recover faster — from a Malaysian physio.

Pelvic Floor After Birth: What Pantang Doesn't Fix
Nearly half of Malaysian mothers experience pelvic floor problems after birth. Pantang helps you rest — but it won't fix leaking, pain, or diastasis recti.

Bahu Beku (Frozen Shoulder): Kenapa Menunggu Memanjangkan Pemulihan Anda
Bahu beku boleh ambil masa 3 tahun tanpa rawatan. Fisioterapi di Petaling Jaya terangkan tiga peringkat frozen shoulder dan kenapa rawatan awal potong masa tu kepada 3–6 bulan.
Book an assessment.
60 minutes. One-to-one with Felicia. Reply on WhatsApp within a few hours.
Message on WhatsApp